CLINICAL RESEARCH
Planned first-line bilateral femoral access for endovascular treatment of unilateral common iliac artery chronic total occlusion: procedural control and outcomes
1
Trabzon Ahi Evren Cardiothoracic Surgery Training and Education Hospital, Trabzon, Turkey
Submission date: 2026-01-31
Final revision date: 2026-04-06
Acceptance date: 2026-04-06
Publication date: 2026-05-13
Corresponding author
Emced Khalil
Trabzon Ahi Evren Cardiothoracic Surgery Training and Education Hospital Trabzon, Turkey
Trabzon Ahi Evren Cardiothoracic Surgery Training and Education Hospital Trabzon, Turkey
Arch Med Sci Atheroscler Dis 2026;11(1):65-71
KEYWORDS
bilateral femoral accessvascular access strategycommon iliac arterychronic total occlusionendovascular intervention
TOPICS
ABSTRACT
Introduction:
Chronic total occlusion (CTO) of the common iliac artery (CIA) represents a technically challenging subset of aorto-iliac occlusive disease, particularly when the lesion extends close to the aorto-iliac bifurcation. Although endovascular therapy has become the preferred treatment modality, the optimal access strategy for unilateral CIA CTO remains uncertain. This study aimed to evaluate the feasibility, procedural control, and clinical outcomes of a planned first-line bilateral femoral access strategy in unilateral CIA CTO.
Material and methods:
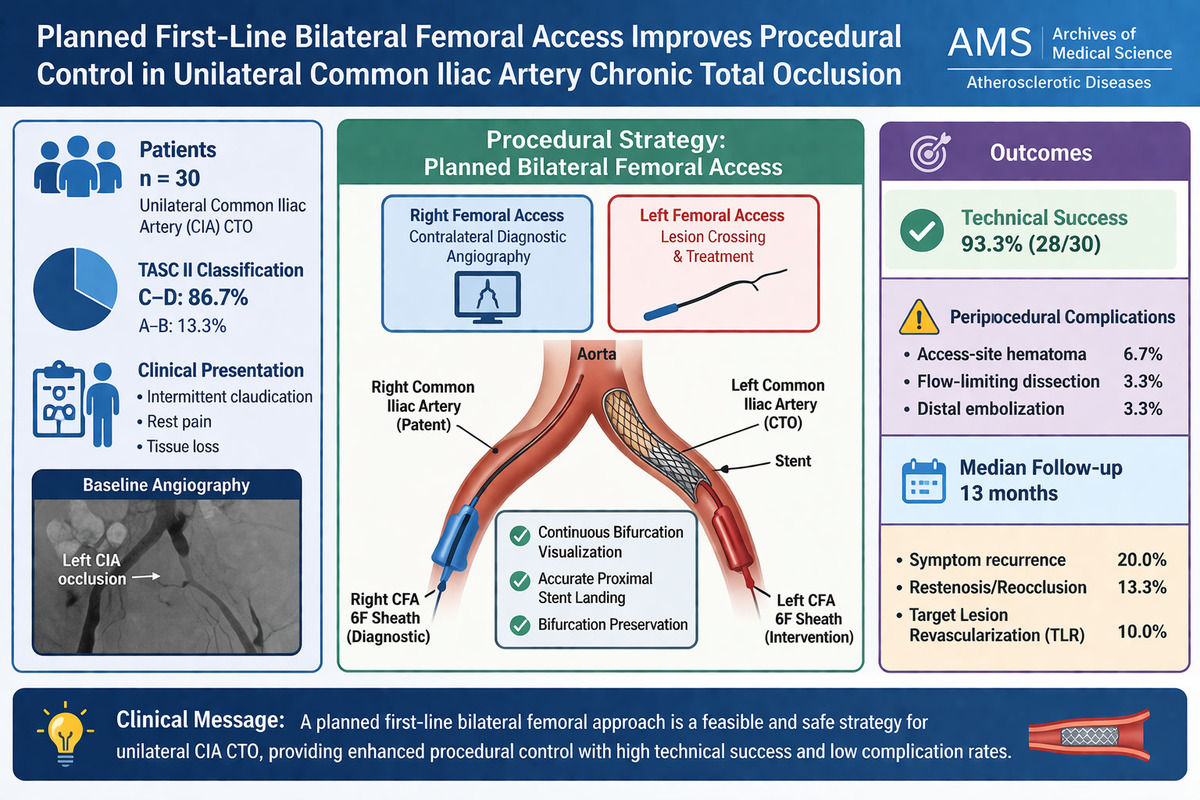
This retrospective single-centre study included 30 consecutive patients with unilateral CIA CTO who underwent endovascular revascularisation using a first-line bilateral femoral approach between January 2020 and December 2024. Continuous contralateral diagnostic angiography was used to guide the lesion crossing and stent deployment. Lesions were classified according to the TransAtlantic Inter-Society Consensus (TASC II). Technical success was defined as residual stenosis < 30% with restoration of antegrade flow. Procedural complications and mid-term clinical outcomes were assessed.
Results:
Most lesions were classified as TASC II C–D (86.7%). Technical success was achieved in 93.3% of cases. Periprocedural complications were infrequent and included access-site haematoma (6.7%), flow-limiting dissection (3.3%), and distal embolisation (3.3%). During a median follow-up of 13 months, symptom recurrence occurred in 20.0% of patients. Imaging performed in symptomatic patients confirmed restenosis or reocclusion in 13.3%, and target lesion revascularisation was required in 10.0% of cases.
Conclusions:
A planned first-line bilateral femoral endovascular approach for unilateral CIA CTO is feasible and safe, achieving high technical success with low complication rates even in predominantly TASC II C–D lesions. By enhancing procedural control and bifurcation preservation, this strategy may be particularly valuable in anatomically complex cases.
Chronic total occlusion (CTO) of the common iliac artery (CIA) represents a technically challenging subset of aorto-iliac occlusive disease, particularly when the lesion extends close to the aorto-iliac bifurcation. Although endovascular therapy has become the preferred treatment modality, the optimal access strategy for unilateral CIA CTO remains uncertain. This study aimed to evaluate the feasibility, procedural control, and clinical outcomes of a planned first-line bilateral femoral access strategy in unilateral CIA CTO.
Material and methods:
This retrospective single-centre study included 30 consecutive patients with unilateral CIA CTO who underwent endovascular revascularisation using a first-line bilateral femoral approach between January 2020 and December 2024. Continuous contralateral diagnostic angiography was used to guide the lesion crossing and stent deployment. Lesions were classified according to the TransAtlantic Inter-Society Consensus (TASC II). Technical success was defined as residual stenosis < 30% with restoration of antegrade flow. Procedural complications and mid-term clinical outcomes were assessed.
Results:
Most lesions were classified as TASC II C–D (86.7%). Technical success was achieved in 93.3% of cases. Periprocedural complications were infrequent and included access-site haematoma (6.7%), flow-limiting dissection (3.3%), and distal embolisation (3.3%). During a median follow-up of 13 months, symptom recurrence occurred in 20.0% of patients. Imaging performed in symptomatic patients confirmed restenosis or reocclusion in 13.3%, and target lesion revascularisation was required in 10.0% of cases.
Conclusions:
A planned first-line bilateral femoral endovascular approach for unilateral CIA CTO is feasible and safe, achieving high technical success with low complication rates even in predominantly TASC II C–D lesions. By enhancing procedural control and bifurcation preservation, this strategy may be particularly valuable in anatomically complex cases.
REFERENCES (18)
1.
Fowkes FG, Rudan D, Rudan I, et al. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet 2013; 382: 1329-40.
2.
Criqui MH, Aboyans V. Epidemiology of peripheral artery disease. Circ Res 2015; 116: 1509-26.
3.
Indes JE, Pfaff MJ, Farber A. Endovascular management of iliac artery occlusive disease. J Vasc Surg 2019; 69: 201-10.
4.
Norgren L, Hiatt WR, Dormandy JA, et al. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J Vasc Surg 2007; 45 (Suppl S): S5-67.
5.
Jongkind V, Akkersdijk GJ, Yeung KK, Wisselink W. A systematic review of endovascular treatment of extensive aortoiliac occlusive disease. J Vasc Surg 2010; 52: 1376-83.
6.
Della Schiava N, Boitet A, Midy D, et al. Endovascular treatment of TASC C–D aorto-iliac lesions: contemporary outcomes. Eur J Vasc Endovasc Surg 2019; 58: 531-9.
7.
Zhang H, Li M, Chen Y, et al. Endovascular recanalization of iliac artery chronic total occlusions: outcomes and predictors. BMC Cardiovasc Disord 2020; 20: 421.
8.
Aboyans V, Ricco JB, Bartelink ML, et al. 2017 ESC Guidelines on the diagnosis and treatment of peripheral arterial diseases. Eur Heart J 2018; 39: 763-816.
9.
Mwipatayi BP, Thomas S, Wong J, et al. Iliac artery stenting and bifurcation preservation: technical considerations and outcomes. J Endovasc Ther 2018; 25: 150-8.
10.
Patel SD, Ganguli S, Walker TG. Dual-access techniques for complex iliac artery occlusions. J Vasc Interv Radiol 2023; 34: 1450-7.
11.
Kouvelos GN, Papas TT, Antoniou GA, et al. Long-term outcomes of endovascular therapy for iliac artery chronic total occlusions. Ann Vasc Surg 2021; 72: 230-8.
12.
Li Y, Zhang X, Wang L, et al. Antegrade versus retrograde crossing strategies for iliac artery chronic total occlusions. Vasc Endovascular Surg 2022; 56: 315-22.
13.
Lakhter V, Aggarwal V. Current status and outcomes of iliac artery endovascular therapy. Curr Cardiol Rep 2020; 22: 98.
14.
Della Schiava N, Midy D, Ducasse E. Endovascular-first strategy for complex iliac occlusive disease. Eur J Vasc Endovasc Surg 2019; 58: 1-3.
15.
Mwipatayi BP, Hockings A, Hofmann M. Prevention of contralateral iliac compromise during iliac stenting. J Endovasc Ther 2017; 24: 123-30.
16.
Leivaditis V, Büki T, Özsoy E, et al. Successful ClotTriever thrombectomy in extensive inferior vena cava and bilateral iliac vein thrombosis with pulmonary embolism. Kardiochir Torakochirurgia Pol 2025; 22: 226-31.
17.
Papadoulas S, Stathopoulou S, Mulita F, et al. Simultaneous endovascular abdominal aortic aneurysm repair and open repair of common femoral artery aneurysm: short case series and current review. Kardiochir Torakochirurgia Pol 2025; 22: 219-25.
18.
Papadoulas S, Kouri N, Tsimpoukis A, et al. Treatment options for dialysis access steal syndrome. Kardiochir Torakochirurgia Pol 2022; 19: 145-50.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.