STATE OF THE ART PAPER
Life-saving but limb-threatening: vasopressor-induced acral ischaemia and necrosis – two cases and review
of the literature
1
Department of Cardiothoracic and Vascular Surgery, Westpfalz Klinikum, Kaiserslautern, Germany
2
Department of Surgery, General Hospital of Eastern Achaia – Unit of Aigio, Greece
3
Department of Surgery, General University Hospital of Patras, Greece
4
Department of Vascular Surgery, General University Hospital of Patras, Greece
5
John Radcliffe Hospital Emergency Department, University Hospitals NHS Foundation Trust, Headley Way, Headington, Oxford OX3 9DU, UK
6
Department of Oncology, General University Hospital of Patras, Greece
7
Department of Orthopedics, General University Hospital of Patras, Greece
8
Department of Surgery, General Hospital of Lamia, Greece
9
Department of Surgery, Spital Herisau, Appenzell Ausserrhoden, Switzerland
10
Division of Cardiac Surgery, Hippokration General Hospital of Athens, Greece
Submission date: 2025-09-28
Final revision date: 2025-12-01
Acceptance date: 2026-01-02
Publication date: 2026-03-30
Arch Med Sci Atheroscler Dis 2026;11(1):38-44
KEYWORDS
amputationnorepinephrinevasopressor-induced ischaemiaacral necrosissymmetrical peripheral gangrenemedico-legal implications
TOPICS
ABSTRACT
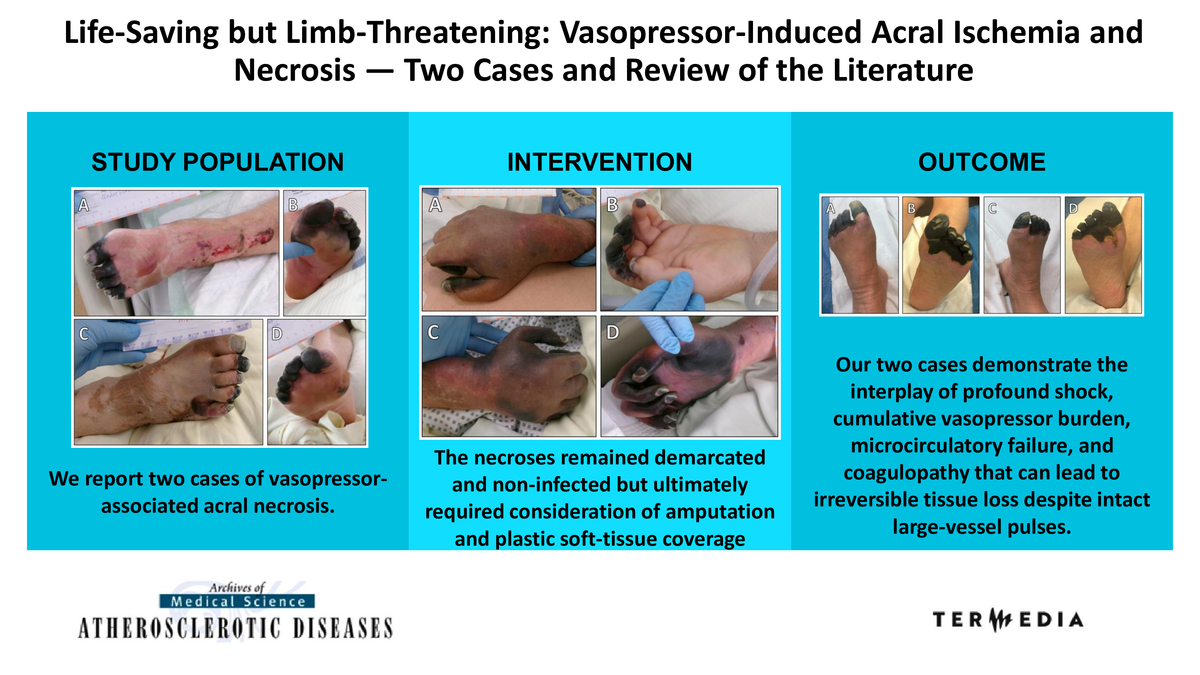
Acral ischaemia and necrosis are rare but severe complications of high-dose or prolonged vasopressor therapy in critically ill patients. Although these agents are life-saving in distributive shock, intense a-adrenergic vasoconstriction, microcirculatory failure, and coagulopathy can converge to cause irreversible digital or limb necrosis, often requiring amputation and sometimes leading to medicolegal disputes. We report two cases of vasopressor-associated acral necrosis. These cases illustrate the multifactorial pathogenesis of vasopressor-induced acral necrosis, in which profound vasoconstriction, endothelial injury, microthrombosis, and the severity of underlying shock lead to distal tissue loss despite intact large-vessel pulses. Consequences include prolonged hospitalisation, the need for staged surgical or reconstructive procedures, long-term functional deficits, and substantial psychosocial burden. The dramatic nature of limb loss after life-saving therapy frequently triggers medicolegal scrutiny regarding dosing, monitoring, and documentation. Awareness of this uncommon but devastating complication is essential.
REFERENCES (18)
1.
Evans L, Rhodes A, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med 2021; 47: 1181-247.
2.
Derry KH, Rocks MC, Izard P, Nicholas RS, Sommer PM, Hacquebord JH. Limb necrosis in the setting of vasopressor use. Am J Crit Care 2024; 33: 226-33.
3.
Daroca-Pérez R, Carrascosa MF. Digital necrosis: a potential risk of high-dose norepinephrine. Ther Adv Drug Saf 2017; 8: 259-61.
4.
Shenoy R, Agarwal N, Goneppanavar U, Shenoy A, Sharma A. Symmetrical peripheral gangrene-a case report and brief review. Indian J Surg 2013; 75 (Suppl 1): 163-5.
5.
Livesey M, Jauregui JJ, Hamaker MC, Pensy RA, Langhammer CG, Eglseder WA. Management of vasopressor induced ischemia. J Orthop 2020; 22: 497-502.
6.
De Backer D, Orbegozo Cortes D, Donadello K, Vincent JL. Pathophysiology of microcirculatory dysfunction and the pathogenesis of septic shock. Virulence 2014; 5: 73-9.
8.
Parmar MS. Symmetrical peripheral gangrene: a rare but dreadful complication of sepsis. CMAJ 2002; 167: 1037-8.
9.
Kwon JW, Hong MK, Park BY. Risk factors of vasopressor-induced symmetrical peripheral gangrene. Ann Plast Surg 2018; 80: 622-7.
10.
Jesani S, Elkattawy S, Noori MAM, et al. Vasopressor-induced digital ischemia. Cureus 2021; 13: e16595.
11.
Ruffin N, Vasa CV, Breakstone S, Axman W. Symmetrical peripheral gangrene of bilateral feet and unilateral hand after administration of vasopressors during septic shock. BMJ Case Rep 2018; 2018: bcr2017223602.
12.
Lu J, Elmarsafi T, Lakhiani C, Sher SR, Attinger C, Evans KK. Septic shock following prostate biopsy: aggressive limb salvage for extremities after pressor-induced ischemic gangrene. Plast Reconstr Surg Glob Open 2017; 5: e1430.
13.
Deldar R, Abu El Hawa AA, Haffner ZK, et al. Achieving functional outcomes after surgical management of catastrophic vasopressor-induced limb ischemia. Plast Reconstr Surg Glob Open 2022; 10: e4175.
14.
Henn MC, Hathaway BA, Lipira AB. Reconstructive surgical management of vasopressor-ischemia related distal extremity loss. J Orthop Case Rep 2025; 15: 45-51.
15.
O’Dell BL, Kochhar K, Johnson A. Vasopressor-induced peripheral gangrene secondary to COVID-19: a case report. J Am Podiatr Med Assoc 2024; 114: 22-216.
16.
Warkentin TE, Ning S. Symmetrical peripheral gangrene in critical illness. Transfus Apher Sci 2021; 60: 103094.
17.
Attallah N, Hassan E, Jama AB, et al. Management of vasopressor-induced acute limb ischemia (VIALI) in septic shock. Cureus 2022; 14: e33118.
18.
Alhumam T, Alhumam AA, Alhumaidi I, Al Rajeh I, Alduhailan Y. Relationship between symmetrical peripheral gangrene patients and using vasopressors in the intensive care unit. Cureus 2024; 16: e58117.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.