Since the initial outbreak of coronavirus disease 2019 (COVID-19) in Wuhan, located in China’s Hubei province, in December 2019, almost 258 million subjects have been infected and more than 5 million subjects have died worldwide, so far [1]. Despite the significant progress in the understanding of COVID-19 pathophysiology and the development of drugs and vaccines against the disease, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) still represents a global nightmare. Coagulopathy due to COVID-19 has been described early after disease identification [2]. Thrombotic events, involving both arterial and venous system, result in multi-organ dysfunction and death in a high proportion of the affected patients [3]. A former prospective autopsy study showed that thrombosis of small and mid-sized pulmonary arteries is found in various degrees in all deceased patients with COVID-19 [4]. Another autopsy study showed the presence of numerous amounts of platelet-fibrin microthrombi in liver specimens obtained from infected subjects with liver involvement during the disease course [5]. Recently, there has been a vivid and ongoing discussion on whether patients with COVID-19 should receive anticoagulation, and if therapeutic heparin regimens are more efficacious for the prevention of surrogate outcomes compared to prophylactic ones. Therefore, we sought to determine the efficacy and safety of therapeutic compared to prophylactic low molecular weight heparin (LMWH) in subjects with COVID-19.
We searched the PubMed and Cochrane Library databases, along with clinicaltrials.gov from inception to 15th February 2022 for randomized controlled trials (RCTs) enrolling adult patients with COVID-19, either hospitalized or outpatients, comparing the efficacy and safety of therapeutic versus prophylactic LMWH. We utilized data from published reports, also searching relevant supplementary appendices for any missing data of specific interest. We excluded case reports/case series, narrative reviews and commentaries (except for research letters). We did not apply any filter regarding study setting or publication language. Two independent reviewers (D.P. and A.D.) extracted the data from the eligible reports. We set as the primary efficacy outcome that of COVID-19 death. We also assessed the following major outcomes: major thrombotic and major bleeding events. Differences were calculated with the use of odds ratio (OR), with the 95% confidence interval (CI), after implementation of the Mantel-Haenszel (M-H) random effects formula. Statistical heterogeneity among studies was assessed using I2 statistics. All analyses were performed at the 0.05 significance level, while they were undertaken with RevMan 5.3 software [6].
Our search yielded 730 results from the PubMed database and 62 results from Cochrane Library. Searching in clinicaltrials.gov did not yield any additional RCT for potential inclusion in our quantitative synthesis. Therefore, we finally pooled data from 8 RCTs in a total of 4817 patients with COVID-19 randomized either to therapeutic or prophylactic LMWH [7–14].
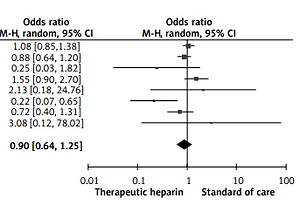
Therapeutic compared to prophylactic LMWH resulted in a non-significant decrease in the odds for COVID-19 death (OR = 0.90, 95% CI: 0.64–1.25, I2 = 52%), as shown in Figure 1. However, therapeutic LMWH was associated with a significant decrease in the odds for major thrombotic events by 45% (OR = 0.55, 95% CI: 0.42–0.71, I2 = 0%), as shown in Figure 2, and a significant two-fold increase in the odds for major bleeding events (OR = 2.12, 95% CI: 1.29–3.49, I2 = 23%), as depicted in Figure 3. Exclusion of the two trials performed in the outpatient setting [9, 14] did not have a significant impact on any of the assessed outcomes. Inspection of the corresponding funnel plot demonstrated asymmetry, generally indicative of the presence of publication bias.
Figure 1
Effect of therapeutic versus prophylactic heparin on the odds for death in COVID-19 patients
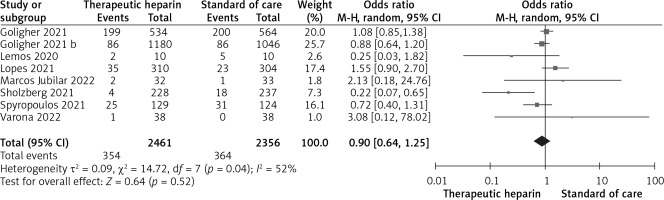
Figure 2
Effect of therapeutic versus prophylactic heparin on the odds for major thrombosis in COVID-19 patients
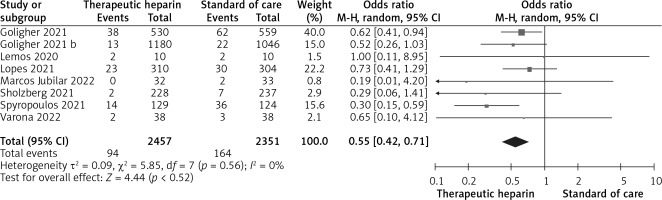
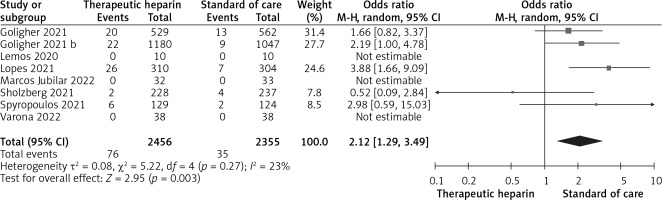
Figure 3
Effect of therapeutic versus prophylactic heparin on the odds for major bleeding in COVID-19 patients
A former meta-analysis of observational studies demonstrated that prophylactic LMWH does not have a significant effect on COVID-19 mortality [15]. In addition, another meta-analysis showed the absence of a favorable effect of anticoagulation on mortality in COVID-19 hospitalized patients [16]. Based on the rather high prevalence of thromboprophylaxis failure among COVID-19 patients admitted to intensive care units, individualized rather than protocolized thromboprophylaxis should be applied [17]. Our pooled analysis of available RCTs addressing the efficacy and safety of therapeutic versus prophylactic heparin in COVID-19 patients showed a neutral effect on mortality, greater odds for preventing major thrombotic events, but at the cost of higher odds for major bleeding events among the enrolled patients. Based on the limited number of available and thus included studies and the presence of ongoing RCTs, we believe that current evidence is insufficient to provide a clear answer regarding this important therapeutic issue. We do agree that treatment should be individualized, after a meticulous assessment of the thrombotic and bleeding risk of the affected subjects, especially those admitted to intensive care units.